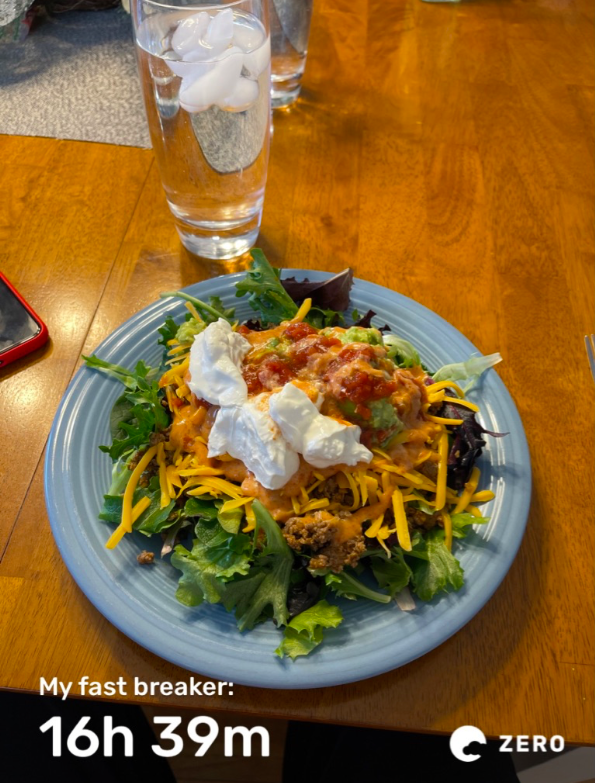I began telling the story of my health journey about 13 months ago on this blog to share what my wife Lisa and I had learned over the previous three years about getting metabolically healthy and losing weight.
We told Lisa’s story of losing at least 40 pounds in July, and followed up in November with her amazing achievement of fitting into her wedding dress for the first time in 36 years. We’re now both down 50 pounds or more from our respective peaks.
Along the way several readers have told us how we had helped to inspire them to try low-carb eating and intermittent fasting. That’s been really gratifying for us, because it’s exactly why we shared our stories in the first place.
So we were particularly happy John Bishop agreed to share his story in August, and that now Rebecca Williams, a colleague at Mayo Clinic, is doing likewise.
Below is Rebecca’s story in her own words. She’s living proof that the standard “eat less, move more” advice is simplistic and ineffective for weight loss in the real world.
And that there is a better way. Here’s what she sent me:
10 years ago, at the age of 41, I ran my first mile with the goal of finishing a marathon. Like many, I really thought that I would lose a tremendous amount of weight by running.
I was wrong. I lost a little, but I was still 60 pounds overweight when I crossed the marathon finish line a year and a half after I ran that first mile. Why was that? I thought I did everything I was supposed to do when running long distance. I carb loaded, I fueled with gels every 30-60 minutes, and since I was burning a tremendous number of calories, I rewarded myself afterwards with pancakes and ice cream.
However, when I step back and objectively assess what I did, I see where I went wrong.

On average, runners burn 100 calories per mile. So, let’s say I’m out for a 15-mile-long run. That means I’m burning 1,500 calories. However, carrying 60 extra pounds meant that 15 miles took me 3-4 hours, and if I was ingesting a 100 calorie gel every 30 minutes, I was taking in at least 600 calories. Then if I rewarded myself with pancakes and ice cream afterwards, that would quickly surpass the additional 900 calories I burned while running. No wonder I didn’t lose weight!
Over the past 10 years I continued running and finished a 200-mile relay, nine half marathons, and countless 5K’s. The weight hung on.
In March of 2020, my husband, Bruce, discovered Dr. Annette Bosworth (a.k.a. Dr. Boz), an internal medicine physician from South Dakota. He purchased her book Anyway You Can, and after reading it he was inspired. The book tells the story of how she saved her mother’s life. Her mother was battling stage IV Chronic Lymphocytic Leukemia (CLL). Facing another round of chemo, her mother decided that she would rather die. Dr. Boz had been studying the science behind the ketogenic diet and was convinced that it would help her mother. The book is the full story of how the ketogenic diet helped her mother achieve optimal health while still battling this chronic cancer. Throughout the book she also explains the benefits of the ketogenic diet.
At the time I was reading this book, Lee Aase started posting stories about his and his wife, Lisa’s, health journey, and I was inspired by them. When I finished Dr. Boz’ book, I was convinced that this is what I needed to do.
Bruce and I took Dr. Boz’ online course, Consistently Keto, and on September 7, 2020 we started our ketogenic journey.
- We reduced our total (TOTAL not net) carbs to <20g per day.
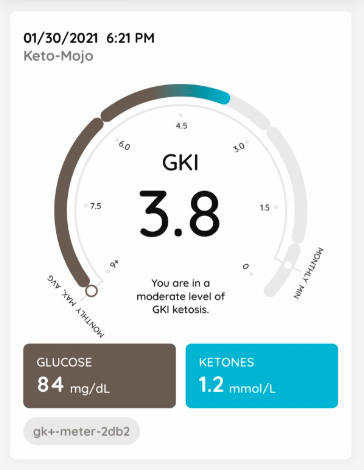
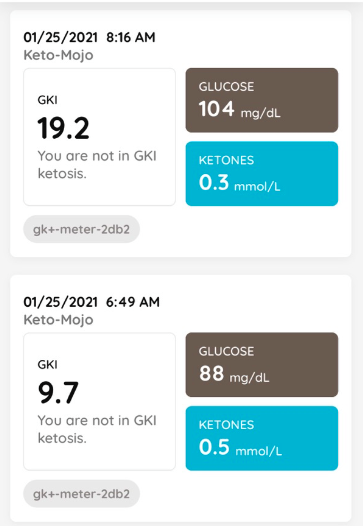
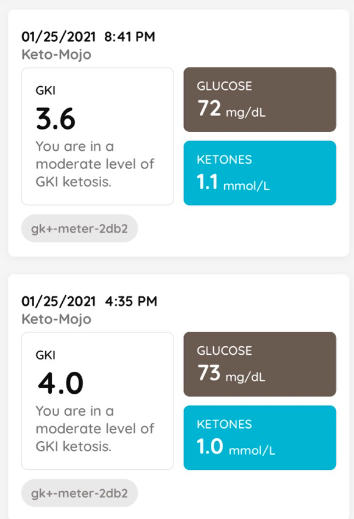
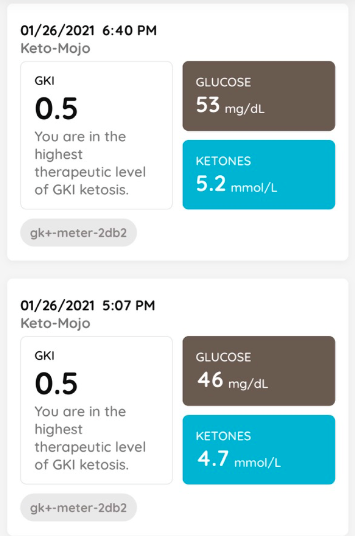
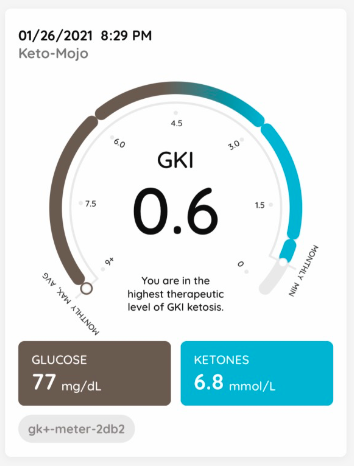
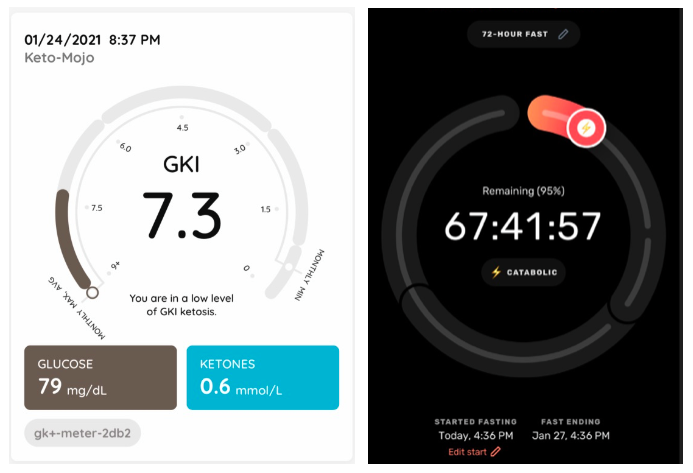
- We measure our urine ketones each morning and use the Chronometer app to track our food and activity.
- I began my day with a bulletproof coffee using a tablespoon of salted ghee and a tablespoon of Brain Octane Oil (MCT). This would keep me satiated until Noon when I at two eggs and 3-4 strips of bacon. I had a half cup of mixed nuts and cheese for an afternoon snack, and dinner was a ribeye steak with creamed spinach.
- As the weeks progressed, I started to incorporate 18:6 intermittent fasting. I dropped the bulletproof coffee and now drink it plain and black. My eating window is from Noon to 6pm.
Since beginning this keto journey, I am rarely hungry, and the sugar/carb cravings are gone. I lost 25 pounds, and I am continuing to run. However, I now run in a fasted state as my body is using my fat for fuel.
I still have 35 pounds to lose in order to reach my goal weight, but I have to say that the ketogenic diet is by far the easiest thing I have ever done and the only thing that has ever worked to help me drop the weight.
I feel amazing! So amazing, in fact, that I am training for my second marathon. In January 2021 I started a couch to marathon training program. The first 12 weeks is training for a 5K, the next 12 weeks are training for a 10K, the next 12 weeks are training for a half marathon, and then the final 12 weeks are training for the Walt Disney World marathon in January 2022. I’m looking forward to this experience allowing my body to burn fat for fuel rather than depend on carbs.
The hardest part of this was making the decision to do it. The easiest part is doing it.
If you have been considering trying low-carb living with intermittent fasting, I hope Rebecca’s story will be that extra nudge that gets you started.
If you have questions about keto or fasting, feel free to ask in the comments below or in my social feeds on Twitter, Facebook or LinkedIn.
If like John and Rebecca you have a story you’re willing to share to help inspire others, send me an email.
I hope you’ll pass along Rebecca’s story with your friends using the sharing buttons below.