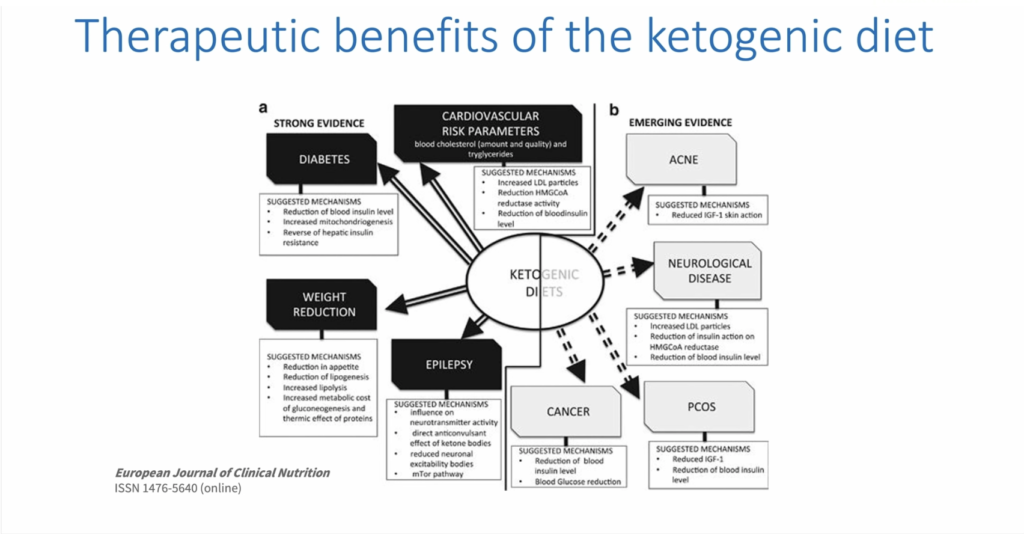
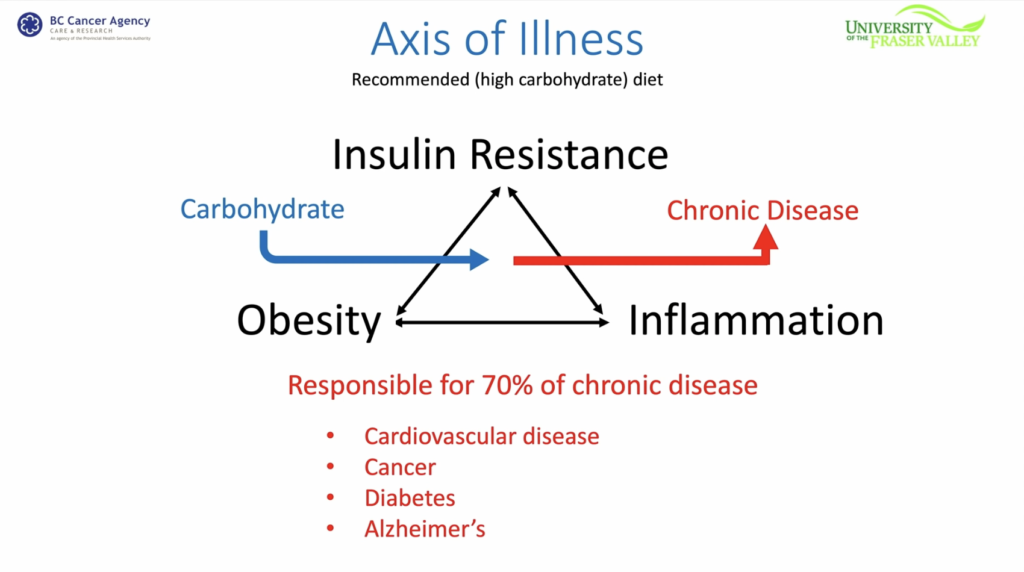
In this video from our friends on the Low Carb Down Under channel, Dr. Paul Mason , one of my Health Sherpas, covers many interesting points. Some of the highlights:
- His personal experience with developing metabolic syndrome, and the relative lack of dietary teachings he received in medical school.
- How medical school teaches doctors to prescribe medications, but not how to de-prescribe medications when patients begin to reverse metabolic syndrome.
- The vegan vs. carnivore dietary controversy, and the relative strengths and drawbacks of each. Both are superior to the standard Australian (or American) diet – or SAD.
- Limitations of nutritional research, including food frequency questionnaires that rely on faulty memories, the healthy user bias and misclassification of pizza, for example, as “red meat.”
- Giving children in Ecuador one egg a day prevented stunted growth. Red meat, dairy and eggs provide the fat needed for brain development in children.
- The strongest experimental design is a blinded randomized control trial (RCT). A meta-analysis gathers related RCTs and re-analyzes them as if they were one larger study. If you see the words epidemiology, association or correlation in the discussion of a study, you should be hesitant to rely too firmly on the results because of possible confounding factors.
- At about the 24:00 mark in the video Dr. Mason discusses environmental issues related to plant and animal-based agriculture, and how grazing animals replenish the soil.
- Cholesterol is essential to human life and is part of all cells. Lipoproteins, e.g. Low-Density Lipoprotein (LDL) and High-Density Lipoprotein (HDL) transport cholesterol through the blood. Starting at about the 40:00 mark, Dr. Mason discusses the bad science behind the saturated fat/LDL hypothesis, and a meta-analysis that showed LDL levels had an inverse relationship to all-cause mortality: the higher your LDL levels, the longer you lived.
- Damaged LDL is the the kind that leads to atherosclerosis, and this damage occurs in two ways: glycation (due to high blood sugar levels, which come from too much sugar and carbohydrates), and oxidation. Vegetable and seed oils are more likely to become oxidized, particularly at lower temperatures.
- The Triglyceride/HDL ratio is a good gauge of whether you have small dense LDL (the dangerous kind, which is called Pattern B), or big, fluffy LDL (Pattern A). This ratio, which you can calculate from a standard lipid panel, is a far better predictor of heart attack risk than LDL cholesterol alone.
- The problem with laboratory test reference ranges is that they reflect results that encompass 95% of the population, so just because your lab results are in the “normal” range doesn’t mean they’re in a healthy range. Much of the population is not healthy.
- High protein and Vitamin D are keys to bone density, and in a study of post-menopausal women and men over 65 those with the highest protein intake actually reversed bone loss.
- Fasting or time-restricted eating are especially helpful for people who are metabolically unhealthy. Even without changing what you eat, you can improve your health by limiting when you eat. (I would add that limiting carbs and becoming fat-adapted makes it easier to limit eating windows.)
There’s lots more, so as you have time I’d encourage you to watch it all. In addition to the points I’ve highlighted above, you’ll hear him drop some truth bombs that you might find jarring because they directly challenge the low-fat, high-carbohydrate orthodoxy promoted by the U.S. government and various medical societies.
An orthodoxy for which the scientific evidence is seriously lacking.
Along with my other Health Sherpas, Dr. Mason’s perspective has helped to reorient my thinking on what is a healthy diet as Lisa and I have been on our health journey over the last few years.
We’ve each lost more than 50 lbs. and have been informally coaching others who have massively improved their health, energy and vitality, with significant weight loss as a welcome side effect.
Based on that experience, I retired in August to launch a new venture we’re developing together with a long-time friend and primary care physician who has had an interest in metabolic syndrome for decades.
We’ll be providing education, community support and coaching to people looking to turn back the clock on their health. Some also will be eligible to take advantage of a direct primary care option.
If you’re interested in learning more, send me an email and I’ll be in touch to give you opportunities for a preview.