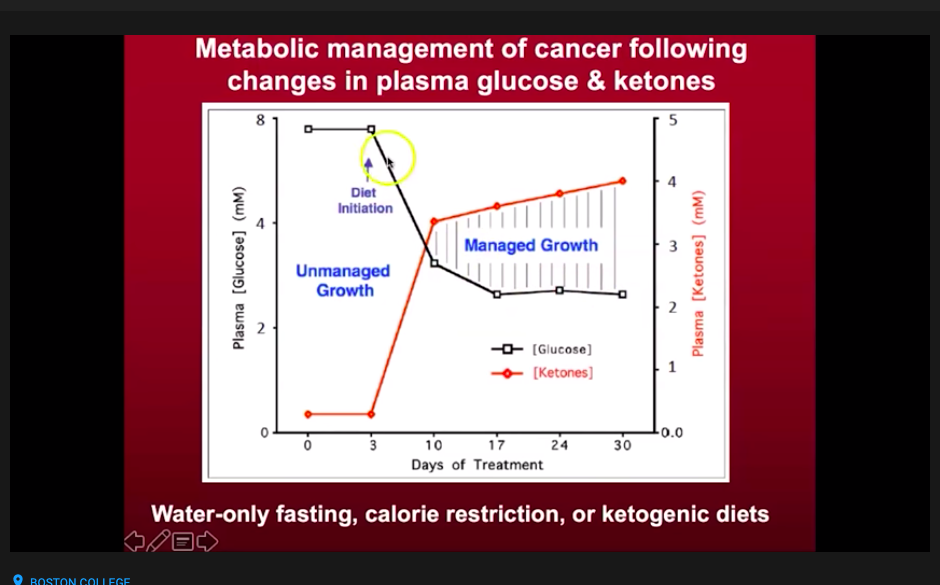
Some thoughts at the end of the second full day of our three-day water-only fast, which we began on Sunday, Jan. 24, as Lisa and I have 15 and 18.5 hours remaining to hit our 72-hour goal.
So far we have been able to stick to the water-only regimen, with a mix of filtered water and mineral water.
We are big coffee drinkers, and were both pleasantly surprised that we didn’t have caffeine-withdrawal symptoms Monday morning. Unfortunately that surprise didn’t last, as the withdrawal symptoms came a little later, as Lisa felt really low in energy and I got a headache in the afternoon and early evening.
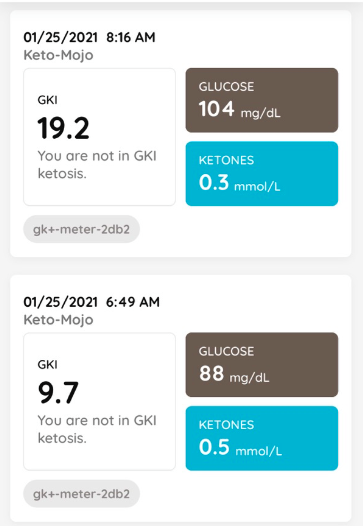
Taking a tip from Dr. Peter Attia, I did an early morning workout on Monday, both bench press and high-intensity rowing. The idea is to burn out the stored glycogen to accelerate the move to fat-burning.
Interestingly, my blood glucose and ketone readings from before and after my Monday morning workout (at right) showed an increase in blood sugar from 88 mg/dL before my workout to 104 after I had showered and settled in to work.
That’s totally normal, and is the result of my liver releasing glycogen for use by my muscles.
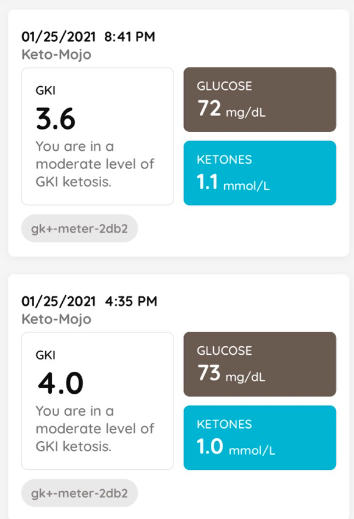
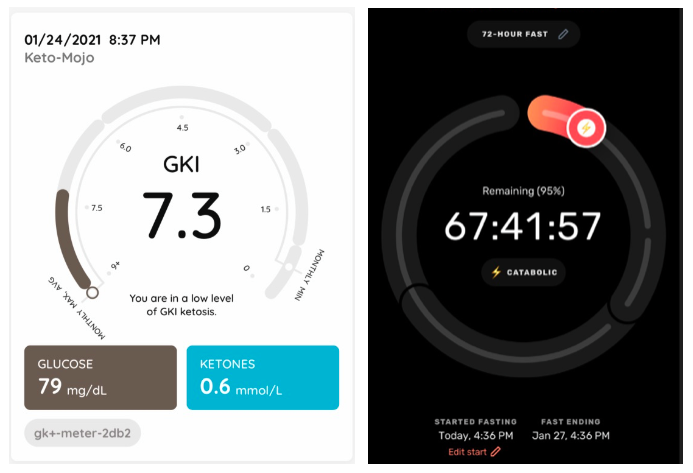
I took readings again at the 24-hour mark of my fast and then at bedtime, which showed that my glucose levels were stabilized due to gluconeogenesis (my liver creating new glucose from amino acids and other circulating substrates), and ketones had begun to climb, reaching 1.1 mmol/L.
With a Glucose Ketone Index (GKI) of 3.6 at bedtime, I was nearing the high level of therapeutic ketosis, but getting there would need to wait until Tuesday morning.
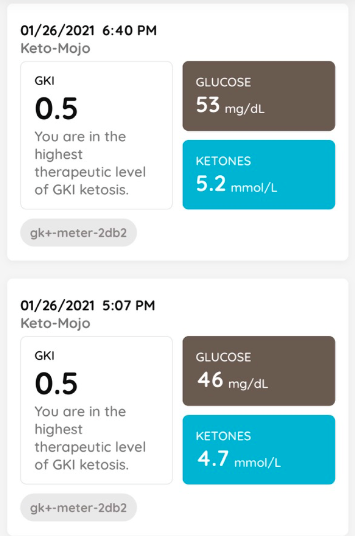
My early morning glucose Tuesday was again 73, but ketones had climbed to 2.2, and by early afternoon those readings were 67 and 4.2, respectively, giving me a GKI of 0.8.
The caffeine withdrawal symptoms were gone, too. We’re supplementing magnesium and salt to maintain electrolyte balances, and mineral water also helps.
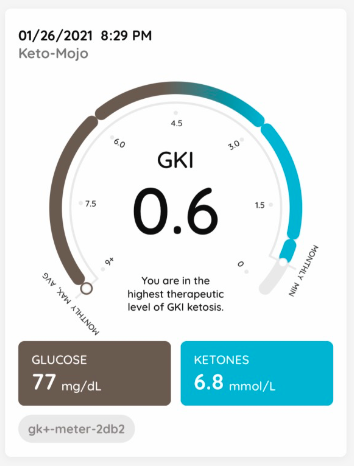
In keeping with Dr. Attia’s advice to do lower-intensity cardio on the second and subsequent days of extended fasts, I waited until after work today to do a 45-minute rowing session. Here were my readings before and after the workout, and at bedtime:
Even though I hadn’t eaten for more than 48 hours, because of gluconeogenesis I maintained adequate blood sugar. And with climbing ketones I have had a GKI under 1.0 for the last nine hours.
I got a Keto-Mojo meter for Lisa, too, and as of this evening she also had reached the 1.0 GKI threshold. Our target is to be below 3.0 for a couple of days, and ideally below 1.0 for a day, for maximum therapeutic benefit.
We’re glad to be in the last several hours of our #3DayCancerPreventionFast. Neither of us would say it has been easy, although we really haven’t felt hungry. Empty is different from hungry. Lisa really misses her coffee, and in future fasts we will likely experiment with allowing coffee, and maybe even coffee with a little cream, and see how our glucose and ketone levels are affected.
I think it’s really helpful having a glucose/ketone meter when doing an extended fast like this. It gives us hard data that what we’re doing is having the desired effect, and when we take readings every few hours we can see the progress.
You may not be able to imagine doing an extended fast for cancer prevention, and if you haven’t done some preparation and adaptation I wouldn’t recommend just diving into it.
Check out My Health Journey for the full story of our health improvements, and my #BodyBabySteps for an approach to how I would do it if I were starting today, based on what I’ve learned.
For us it seems like a worthwhile investment in our long-term health, and I’ll share tomorrow’s experience including breaking our fasts in my next post.