I’m pleased to announce, now that I have retired from leading Mayo Clinic’s social media program, that the third career I’m starting today will build significantly upon that experience.
I am affiliating with Jarrard Phillips Cate & Hancock, a Top 10 communications firm nationally and one in which my good friend and colleague Reed Smith is Vice President, Digital Strategy. Here’s the news release and my profile on the Jarrard site.
As I discussed with Reed and Chris Boyer in the touch point podcast released this morning, the of counsel role with Jarrard will give me an opportunity for continued thought leadership as well as engagement in interesting projects on behalf of clients.
That role also will give me flexibility to pursue another project that is a personal passion for Lisa and me: helping people restore their metabolic health.
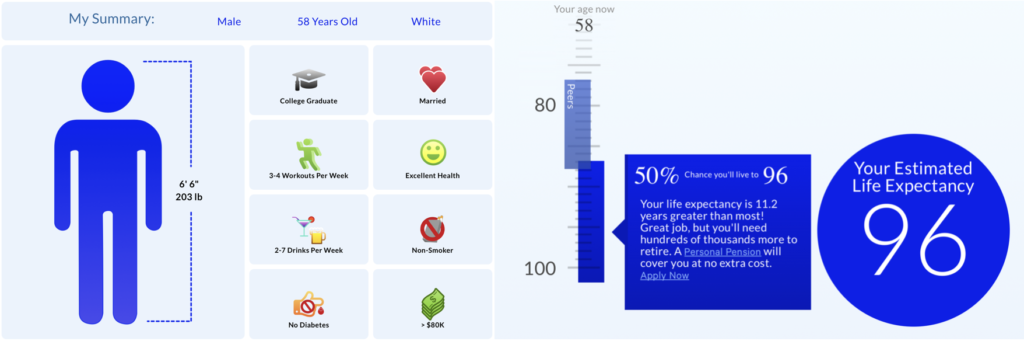
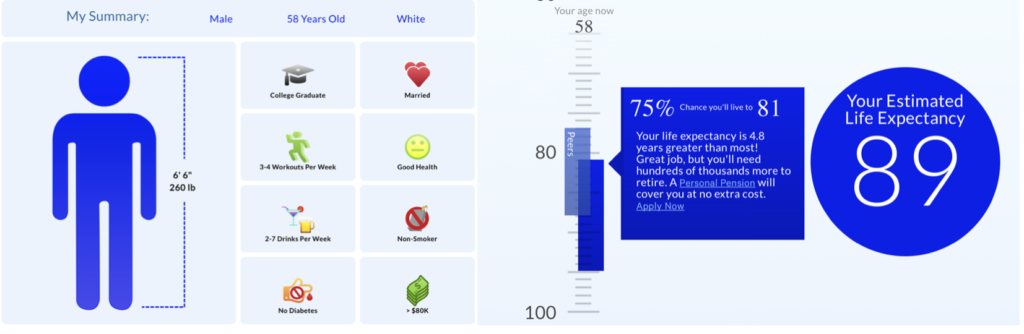
Those who’ve been following my blog and social media accounts will know that Lisa and I have been on a health journey for the last four years.
We’ve each lost more than 50 lbs. and have kept it off. More importantly, we feel healthier and have more energy than we did 20 years ago, and our medical lab test results attest to our restored health.
Since I have been blogging about My Health Journey, Lisa and I have had opportunities to do some informal health coaching with interested readers, and they’ve gotten significantly positive results, too. My #BodyBabySteps page has some of the highlights of our approach, which we are further refining in partnership with a family physician friend.
We want to be able to expand this to reach and help more people, and we’re developing a venture to do just that.
We want to help people turn back the clock on their health.
Maybe even feel healthier than they can remember.
We aren’t ready to announce the venture yet, but in addition to my Jarrard work we will be busy working out the program details in the coming months.
Let’s just say in addition to coaching we will have an online community component, so my social media experience will be important in this part of my third career as well.
If you’re interested in being one of our early participants to help us formulate the program, send me an email and we can discuss.
Be well.